In this article, I want to share a design I have created for a “Pop up Covid-19 Vaccination Clinic” Its based on the practices as used by the NHS in England. The design is flexible and can be modified to suit local clinical regulations. My focus is on technical infrastructure. If anyone uses the draft information below, its essential to use these plans as inspiration and involve clinical experts in the final design to be deployed.
The Site Plan
The site has been designed to facilitate the smooth flow of people through a one way system. Markings will be placed on the floor to remind patients to maintain the correct social distance. A waiting area is provided outside where patients can queue and have their temperatures checked. With good planning, appointment slots can be given to patients so that they arrive at specific times to prevent overcrowding at the entrance. Before entry, the temperature of each patient will be checked.
This is a “pop-up” clinic which means that it needs to be built quickly and brought into service. The modules in the plan can either be tents or temporary structures made from local materials such as plastic sheeting and timber.
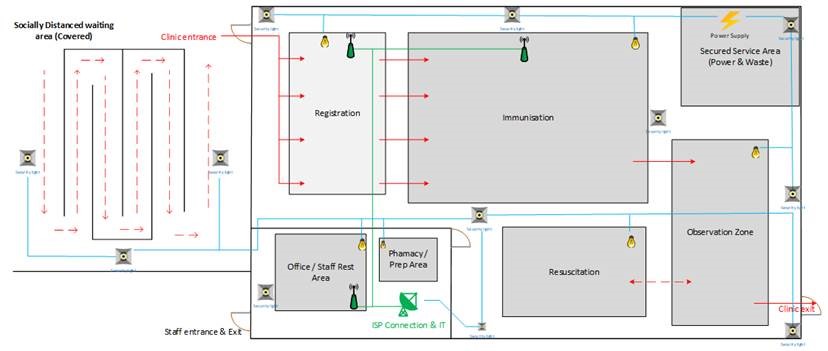
Once inside the clinic, the patient is registered on the appropriate IT system which is defined by the country government where the vaccinations are taking place. Some vaccines will require a second future dose, so accurate record keeping and recording of patient contact details will be essential. Screening can also be managed at the registration post. Any patients who fail screening for reasons such as previous reactions to vaccines can be taken out of the clinic via a side entrance.
The next stage is vaccination. This site has been designed to support 8 clinical bays, so it is possible to have a daily throughput of 600+ patients if the clinic is open for 12 hours a day. Good HR planning is essential as there should be sufficient staff to allow for breaks. In hot countries larger teams may be needed as the time staff can spend in full PPE will need to be limited.
After immunisation, an observation area is provided if its needed for the vaccine being administered. In the UK, the Pfizer vaccine is using new techniques and as a precaution, patients will stay in the observation zone for 15 minutes. If there has been no reactions to the vaccine, the patient will be free to leave. Should there be a severe reaction such as anaphylactic shock, the resuscitation module is set up where the patient can be managed.
The whole clinic is secured with fencing. Inside the clinic, there are two restricted areas where access is limited to staff only. A main service area is used to host the pharmacy and staff office / rest room. Another secure area is set up to host power generation and waste management.
Other modules can be added to the staff zone such as wash rooms and PPE storage.
ICT
The basic IT will consist of an internet connection such as 3G or satellite for remote areas. Secure Wi-Fi hotspots will be set up for the computers and if resources permit, public Wi-Fi can be used to provide patients with information. The software used to manage patient information will need to be determined locally in each country. Its likely to be a government system.
Clinical Waste Management
Waste from the clinic needs to be handle carefully and responsibly. Firstly items of PPE may need to be incinerated so that the risk of contamination is removed. The empty containers which held the vaccine must either be returned to a formal system to recycle the containers or they must be destroyed. The containers must not fall into public circulation as they may be used by criminal gangs to make money from fake vaccines.
Cold Chain
Vaccines must be stored in a medical standard fridge. The specific model of fridge will be determined by the sort of vaccine in use and its environment requirements. As part of the clinic design, there needs to be stable power available for the fridge with back-ups. If power fails, this might result in temperature levels rising which will destroy the vaccine. The following design concept should be sufficient to mitigate this risk.

The power source will either come from the local grid or generator. An Inverter/Charger is provided and will charge batteries while power is available. Should the power fail, the battery will take over and power the fridge via the inverter. The battery bank will be sized to provide power for at least 24 hours. The Inverter/Charger has built in IOT technology and will send an alert to let management know that power has failed. (Note – core IT infrastructure will also be connected to the same back up power supply).
As a further protection, a smart temperature sensor can be added to the fridge to monitor temperature and send alerts when temperatures are close to becoming too high or too low.
Conclusion
This is a very high level design. There will be various clinical factors to be added. Other modifications may be needed to make the site accessible to disabled patients. This design is a good starting point for a team of experts to begin work.
